Today is the first in a series covering what it’s like to return to rugby from a major injury. It was motivated by our friend Clarke Cayton’s two-part series on returning to rugby from a broken leg.
If you’ve returned to rugby from a major injury and would like to be paid to share your story, we’d love to hear from you! Please email get@ruckscience.com.
There is no one to blame for my ACL injury but myself. People tell me it was bad luck or bad timing or both. The truth is that it was my fault and I could have avoided the injury or at least I could have minimized the risk of it happening to me.
I know I had let my prehab and rehab exercises slip.
I got a little bit busier with work and a little bit less concerned with the important little things I had learned as a professional player. The years of work on a Rugby fit body and injury free seasons were slipping every day as I lost my focus on preventative training. Now? I’m another in the long list of rugby players who have torn their ACL.
ACL injury. The anterior cruciate ligament (ACL) is one of the key ligaments that help stabilize your knee joint. The ACL connects your thighbone (femur) to your shinbone (tibia). It’s most commonly torn during sports that involve (1) impact to the knee, sudden stops and changes in direction.
Returning to rugby from any injury requires time, dedication and a commitment to getting better. ACL injuries seem to have become more common in recent years. Though it’s also possible that they’re also just being diagnosed more accurately. Some of the specific challenges I encountered when attempting to recover from my ACL injury included:
There are many reasons why we tear or rupture our ACL. Approximately 75% of ruptures are sustained with minimal or no contact at the time of injury. Sidestepping is the typical mechanism that causes the ACL to tear, that being a sudden change in direction or speed with the foot firmly planted. A direct blow to the side of the knee, hyperextension of the knee or quickly changing direction, landing from a jump or turning. Chances are you know someone who has done it.
I was playing club rugby and made a break on the short side. One big step off the left foot to accelerate, possibly uneven ground, muscle fatigue or instability in the knee and… POP! Caught in the open field by a sniper on the grandstand roof, is how my imagination replays the incident. I was in open space without a single player around me, and suddenly I collapsed into a heap on the ground. Absolutely devastated.
I knew that it was something wrong. After years of playing rugby, I knew that my ACL was in bad shape. That haunting popping sound happened in my knee, which many teammates had described before. As weird as it seems, at that moment my knee gave way I could imagine the anatomy of my knee and the rupturing of the ligamentous fibers. Our physiotherapist tried to reassure me, “It might not be that bad,” however, I knew it was. There was a lot of pain for about two minutes, calming into a dull ache and then strangely only limited swelling, which is uncommon for most people .
Everyone experiences something different and sometimes you do not even know you have done it, thinking you can play on. However if you can play on (which I would strongly advise against), the knee is put under more pressure as there is instability and further damage can be done. The dreaded popping sound typically only means one thing. A tear or rupture.
The worst part about an ACL injury is not even the physical aspect or even the pain. It is when the mind starts making the injury worse than it actually is. All types of crazy thoughts and questions come rushing into your head. For example:
At one point I thought I was just making it up because most of the pain dissipated quickly. In reality when things settle and more importantly your mind settles you can tackle the task ahead whatever the outcome. A lot of people have recovered from much worse injuries or accidents and shown a recovery that resembles that of Wolverine in X-Men. Professional Rugby Players who have successfully recovered from an ACL injury to play top-level rugby again include; Jonathan Davies, Rhys Webb, Jamie Roberts, Alex Dunbar, Quade Cooper, Aaron Cruden.
Science and Technology are improving every day. Research is being done on people who are hyper flexible and using different methods to repair the ACL. For example using other people’s tissue or animal tissue for better surgical results.
Bridge Enhanced ACL repair. The new technique, bridge-enhanced (TM) ACL Repair (BEAR(TM)), uses stitches and a bridging scaffold (a sponge injected with the patient’s blood) to stimulate healing of the torn ACL providing a quicker recovery and fewer complications in later life.
Incorrect training techniques and form has lead to an increase in lower leg injuries. In general, we live a more sedentary lifestyle which has an effect on health, mobility and athletic performance.
It is important to understand the stats and how common ACL injuries are. Annually there are around 200,000 ACL injuries. Over half of these need reconstructive surgery.
Firstly stay positive. There is no good drowning your sorrows and making decisions about the future of your rugby career until you have all the information. Many players have overcome the injury. If you are a professional player use all your resources, medical teams, and players associations to get the best results. If you are an amateur, I hope you are covered by ACC (if in New Zealand), or you have insurance. If you have none of the above here is some info for you.
Managed swelling with ice, got a comprehensive diagnosis, MRI and consult with a specialist knee surgeon. Worked on movement and strength exercises as much as possible to help the knee before surgery. Tried to stay positive, as I thought I might never play Rugby again. Pitchside treatment is difficult to remember, to be honest, I was not actually listening to our physiotherapist. A typical test a physio might use to test your ACL is the Anterior Drawer Test.
However, swelling can make the knee act like there is an end point in the ACL. (Endpoint meaning it is still attached and not completely snapped.) Managed any swelling with ice. I got a comprehensive diagnosis with an MRI and consulted with a surgeon. Worked on movement and strength exercises as much as possible to help maintain strength prior to surgery. I was scheduled for a surgery which would take a piece of my hamstring, and that would be used as the new ACL after the broken one was removed and cleaned up. This is called a Graft. There are three common types of graft harvest sites: Patellar tendon, hamstring tendon, quadriceps tendon (4).
Further research into injury, planning and goal setting with physiotherapist and surgeon.I actually missed my pre-surgery appointment. This is good to go to so you can ask as many questions as possible and they check all your vitals. To get around this, they agreed to look at my blood pressure before the surgery. They would have canceled my surgeon if I was not in good health.
Hamstring graft, left knee reconstruction.
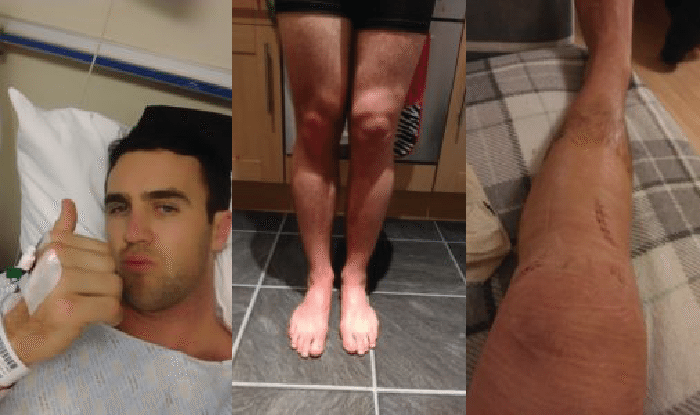
Note the amount of swelling around the knee and atrophy of the quadriceps only a few days after surgery.
Basic movements, quad activation, stitches, and staples out after 10 days. Walking with crutches with the focus on getting the correct walking gait. 3-5 times a day 10-20 steps. Walking backward helped a lot as well. Some of the exercises I found most useful for ACL recovery were:
This is where I continued to work on the exercises above. I also added in some exercises designed to correct imbalances and to develop strength-endurance. I also added extra prehab – rehab exercises for the rest of my body to fix any other niggles. To correct imbalances I did more single leg work on my injured leg compared to good leg.
Firstly I worked on range of movement and correcting any imbalances in the body. (notable differences in both legs and core strength). After correcting imbalances, I focused on muscular endurance. This phase was lighter weight or theraband and higher reps of 10-15, x 3 sets. Having a lighter weight allowed me to focus on movement and get the knee working longer. Once I had a sufficient amount of time 6-8 weeks of higher reps I cycled in a strength phase using a rep range of 2-3reps with heavier weights and longer rest 2 minutes -3 minutes between sets. After further gains, I followed up with a mass building block working to reps of 5+ or failing at the 5th rep.
Using a heavy weight and a tempo of 5 seconds down, hold for 2 seconds, 5 seconds up. It took a long time after the operation to regain full strength, so I was still much weaker in the left leg. To help build the muscle up I did mostly single leg exercises to failure and to make the recovering leg work harder I used my other leg to help push more reps out with double leg exercises. For example the quad extension exercise machine. With a heavier weight, it was difficult to complete the full range, so I worked the muscle at different points in the range and held for a 5 second to 10 seconds. This was then repeated. Endurance, strength then Mass. Still doing a lot of cycling, swimming and running in the pool.
There is no clear time frame, so it will be different for everyone, but this is where I was. A good tip is to measure your success and improvement by month. This helped me with my mindset and always showed an improvement even if each week it was hard to see. I was still doing a lot of the same exercises in stage two as stage three. The leg will regain enough mass and will have a noticeable improvement in strength giving you the confidence to increase your training. I was feeling strong enough to start jogging.
Here is a program I did in the first few weeks of running. Return to running. You can be overwhelmed with everything that needs to be done however do not use this as an excuse to do nothing. Depending on your goals or your own personal weaknesses you must tailor your training regime to suit. I felt at one point my quadriceps were working well, but I needed to add in more hamstring work. The best exercise I can recommend to develop hamstring strength are the Nordic drops or swiss ball hamstring curls. Romanian deadlifts and single leg Romanian deadlifts.
As you make the decision to return to rugby, it’s vital that you continue performing your strength exercises but working in more dynamic movements and on multi-directional planes. This is where the knee should be at 90-100%. You can start to build in sport specific exercises and more power work. Continue balance and proprioception work – benchmark standing on one leg with eyes closed for over a minute.
Key Points
Gradually build into Rugby training. Avoided contact early on and add some bits of contact in each week to build confidence. Complete at least two full weeks of training without contact and two full weeks of training with light contact.
Game 1 – Started played 55 minutes – Struggled with match fitness and hamstring tightened up just after half time. Should have just played 40 minutes.
Everyone should have their own specific injury prevention program. It should be position specific as many of the injuries we get as rugby players are position specific. For example, Props have a higher rate of spine and neck injuries and disc problems due to the forces in the scrum. As a fly-half your a more susceptible to hamstring injuries and groin injuries due to higher amounts of kicking and sprinting.
Below is my small Pre-hab/Rehab program to add into your program to help avoid injury. Proper screening and testing should be done on your own body to have the best outcomes however here is a basic injury prevention program to add into your strength and conditioning.




While lying on side with your spine in neutral, hips stacked on top of each other and a 45-degree angle at the hip joint kip leg straight up and lower slowly and controlled. This is progressed to holding the foot in the elevated position and moving the foot in small forwards circles ensuring the movement occurs at the hip.
Several of these were covered in the recent article covering exercises to master breakdown poaching. The weighted crawl is a good one. Check that article and the video to get the low down.






Swimming, walking and stretching in a cold pool Light 20-30 minute bike ride or stationary cycle in the gym Ice baths or intermittent hot and cold exposures finishing with cold. Good Nutrition – Foods to help fight inflammation for Rugby players are oily fish or fish oil tablets (make sure they are good quality), Blueberries, Beetroot, nuts, leafy greens, garlic, turmeric, ginger, and tomatoes.
Have you experienced an ACL injury playing Rugby? What was the best exercise you did or have been doing to prevent knee injuries or other injuries? We welcome your questions comments and recommendations to help rugby players who have suffered an ACL injury to return to rugby.
We design & manufacture premium nutritional supplements specifically for the rugby community. Our range of supplements can help professional and amateur rugby players alike to perform, recover and live better.
The materials and information provided in this presentation, document and/or any other communication (“Communication”) from Ruck Science, LLC or any related entity or person (collectively “Ruck Science”) are strictly for informational purposes only and are not intended for use as diagnosis, prevention or treatment of a health problem or as a substitute for consulting a qualified medical professional. Some of the concepts presented herein may be theoretical.
References to any non-Ruck Science entity, product, service, person or source of information in this or any other Communication should not be considered an endorsement, either direct or implied, by the host, presenter or distributor of the Communication. The host(s), presenter(s) and/or distributor(s) of this Communication are not responsible for the content of any non-Ruck Science internet pages referenced in the Communication. Ruck Science is not liable or responsible for any advice, course of treatment, diagnosis or any other information or services you chose to follow without consulting a qualified medical professional. Before starting any new diet and/or exercise program, always be sure to check with your qualified medical professional. For details of our affiliate program please see our Terms & Conditions. Click here for our Privacy Policy